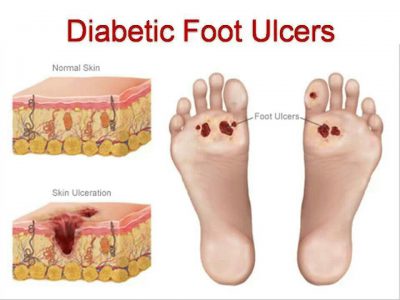
DFU(Diabetic Foot Ulcers)
Diabetic foot ulcers occur as a result of various factors, such as mechanical changes in conformation of the bony architecture of the foot, peripheral neuropathy, and atherosclerotic peripheral arterial disease, all of which occur with higher frequency and intensity in the diabetic population.
Nonenzymatic glycation predisposes ligaments to stiffness. Neuropathy causes loss of protective sensation and loss of coordination of muscle groups in the foot and leg, both of which increase mechanical stresses during ambulation.
Diabetic foot lesions are responsible for more hospitalizations than any other complication of diabetes. Diabetes is the leading cause of nontraumatic lower extremity amputations in the United States, with approximately 5% of diabetics developing foot ulcers each year and 1% requiring amputation.
Physical examination of the extremity having a diabetic ulcer can be divided into examination of the ulcer and the general condition of the extremity, assessment of the possibility of vascular insufficiency, and assessment for the possibility of peripheral neuropathy.
The staging of diabetic foot wounds is based on the depth of soft tissue and osseous involvement. A complete blood cell count should be done, along with assessment of serum glucose, glycohemoglobin, and creatinine levels.
The management of diabetic foot ulcers requires offloading the wound by using appropriate therapeutic footwear, daily saline or similar dressings to provide a moist wound environment, debridement when necessary, antibiotic therapy if osteomyelitis or cellulitis is present, optimal control of blood glucose, and evaluation and correction of peripheral arterial insufficiency.